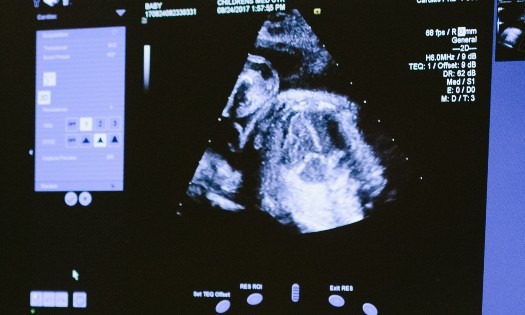
In August 2021, a baby girl with a prenatal diagnosis of congenital diaphragmatic hernia (CDH) was born at a hospital in North Texas. The imaging she had prior to birth showed a left-sided CDH, which meant there was a hole in the muscle that separates the chest from the abdominal cavities on the left side. A large volume of the organs from her abdomen was in her chest cavity, including intestines, spleen and part of the liver. This caused her lungs to be underdeveloped. Immediately after birth, she was stabilized with mechanical ventilation and fluids, and then she was transferred to the Level IV Neonatal ICU (NICU) at Children’s Health℠ in Dallas.
Our dedicated multidisciplinary team treats and manages these babies born with complex surgical conditions using advanced techniques, such as minimally invasive surgical approaches. This particular baby’s case was even more complicated, as she weighed only 2.28 kilograms in combination with a very large hernia defect.
“If thoracoscopic repair can be performed safely, that’s the option we move forward with since it is associated with decreased pain, and it could also minimize time on mechanical ventilation post-surgery,” says Mark Ryan, M.D., Pediatric General and Thoracic Surgeon at Children’s Health and Assistant Professor of Surgery at UT Southwestern. “Our depth of experience, technology and multidisciplinary collaboration allows us to take on even the most complex conditions and perform minimally invasive procedures within the smallest operating space, like we did for this baby girl.”
Multidisciplinary Assessment for CDH
Our multidisciplinary team, including a neonatologist and pediatric surgeon, worked closely with the patient’s family and referring provider before birth to review imaging and discuss possible treatment plans.
“Babies with CDH face a mortality rate exceeding 30%, mostly because the condition compresses the lungs and heart, causing many difficulties for newborns to sustain critical lung functions,” Dr. Ryan says. “Our team reviewed a fetal MRI before birth, which indicated the baby would likely have reasonable lung function and wouldn’t need advanced respiratory support. This also meant that thoracoscopic repair could be an option but, of course, that always depends on the baby’s condition after birth.”
When the baby arrived at Children’s Health, she remained stable with mechanical ventilation and didn’t require more invasive support, such as extracorporeal membrane oxygenation. A team of specialists from pediatric surgery, cardiology, radiology and anesthesiology began a thorough evaluation to determine the best treatment plan.
“The thoracoscopic repair procedure involves blowing air into the chest at a low pressure, which further compresses the lung and heart,” Dr. Ryan explains. “This baby had sufficient lung capacity for the procedure to be safe from that aspect, but we needed further studies to assess heart function and determine if there were any other related anomalies, which frequently occurs in CDH patients.”
Together, the multidisciplinary team determined that a thoracoscopic surgery could be performed safely.
Operating with Four Millimeter or Smaller Incisions
Children’s Medical Center Dallas is designated as a Level I Children’s Surgery Center by the American College of Surgeons, and we treat more pediatric patients with minimally invasive procedures than any other hospital in the region.
“If we had done this procedure open, the incision would go from the middle of the abdomen to the far left side of the body,” Dr. Ryan says. “Instead, we had three incisions of four millimeters or less. The operating space for an infant that size is approximately one hundred cubic centimeters, which is about half the size of an orange. With our 4K high-resolution thoracoscopic camera system, we’re able to safely perform the procedure in this small space and maintain visualization of vital structures.”
Before closing the hole in the diaphragm, the team pushed the organs from the abdominal cavity down and manipulated them into the correct place with tiny three-millimeter tools. Then Dr. Ryan measured the hole.
“The defect was about three centimeters wide by six centimeters long. Because there weren’t enough of her native diaphragmatic muscles to close the defect, we used a patch. This wasn’t easy since it requires delicate surgical techniques in such a small cavity,” Dr. Ryan explains.
After the two-hour procedure, the baby returned to the NICU for recovery.
Better Outcomes and Faster Recovery
The baby was extubated after two days, which is below the average number of days on mechanical ventilation for babies who undergo CDH repairs. Her postoperative recovery was uneventful with a relatively short NICU hospital course.
She was discharged home with the support of our THRIVE Program, which provides specialized follow-up care for high-risk babies.
“At her one-month check-up, we did a follow-up chest X-ray, which showed her fully expanded lungs on her left chest, and she looked great,” Dr. Ryan says. “She’s breathing normally and tolerating a diet without any issues.”
This baby’s story is just one example of how our multidisciplinary team is ensuring the best outcomes for the most complex surgical cases.
“We have the specialists, expertise and technology to treat every condition,” Dr. Ryan says. “That enables us to comprehensively evaluate treatments for complex conditions, like thoracoscopic versus open repairs for CDH, and identify how we can continue to improve care for these children.”
Learn more about innovative surgical care at Children’s Health and how to refer patients >>