It’s no secret that pediatric neurosurgery is evolving rapidly. The challenge is finding effective ways to incorporate new technologies and approaches into real-world pediatric practice – especially when they were first developed for adults.
Bradley Weprin, M.D., Pediatric Neurosurgeon at Children’s Health℠ and Associate Professor of Neurosurgery, Pediatrics and Radiation Oncology at UT Southwestern and his colleagues take that challenge head-on and are among the first pediatric neurosurgery teams to offer everything from MRI-guided laser ablation to interventional neuroradiology techniques. Here are four ways we’re using new advances to reshape care:
Combining SEEG and ROSA for Precision Diagnosis
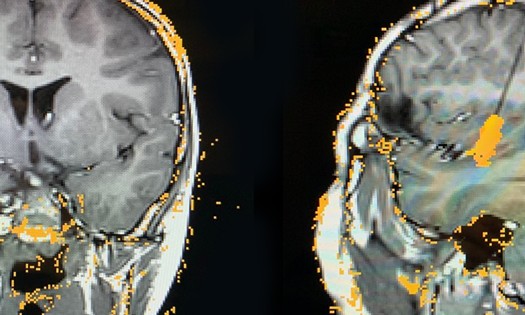
Surgery can be highly effective at controlling epilepsy when medications fail. But families and some referring physicians are daunted by invasive diagnostic procedures and neurosurgeries. Dr. Weprin’s team was an early adopter of stereoelectroencephalography (SEEG) for children and adolescents, and we recently added the Robotized Stereotactic Assistant (ROSA) to the Children’s Health surgical suite, after several years of using it at UT Southwestern.
“SEEG significantly increases coverage of the brain, which means we can pinpoint seizure onset zones with much greater accuracy,” says Dr. Weprin, who serves as the Division Director of Pediatric Neurosurgery at Children’s Health. He is also Vice-Chair of the Department of Neurological Surgery and Director of Pediatric Neurosurgery at UT Southwestern.
What’s more, ROSA reduces surgery times by half, and spares many kids from invasive grid and strip placement.
“SEEG has been just as effective as intracranial surgery, and patients have shorter recovery times and get back to normal activities much faster,” says Angela Price, M.D., a colleague of Dr. Weprin who specializes in surgical epilepsy. “That means more and more potential candidates are going to be referred for these procedures, and that many of those patients are going to overcome their seizures without taking medication for the rest of their lives.”
Expanding the Boundaries of Laser Ablation
The team at Children’s Health and UT Southwestern is building on this progress by exploring ways to apply laser ablation to deep-seated brain tumors and other pathologic entities like cavernous malformations.
“We think the laser could give us the ability to resect deep-seated lesions and address vascular abnormalities that were previously deemed untreatable,” Dr. Weprin says. “It could open the door to treatments for kids who are running out of options.”
Incorporating Interventional Neuroradiology into Practice
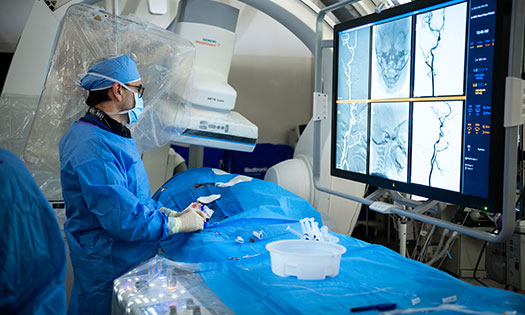
Interventional neuroradiology techniques – like endovascular coiling and embolization – have become commonplace in adult treatment, but there are only a small handful of specialists who have experience applying them to pediatric patients. That’s why we recently recruited Rafael Sillero, M.D., to our team.
Dr. Sillero is a pediatric neurosurgeon with advanced training in interventional neuroradiology. He is experienced in angiography and a variety of other innovative techniques that set him apart from his peers.
“Dr. Sillero is going to be our sixth surgeon, and his presence will significantly expand the minimally invasive options for stroke and many other conditions,” Dr. Weprin says.
Using Outcomes Research to Improve Care
We’re also using a state-of-the-art data platform to interrogate our practices and find ways to make them more efficient.
For example, we analyzed our Chiari decompression practices and found that all of our surgeons have nearly the same results, even though they each do the procedure differently. This revealed ways to standardize our protocols to reduce O.R. time and lower costs.
For instance, we had always sent Chiari decompression patients to the ICU after surgery. But our analysis showed that it had been more than 18 years since one of our patients had a major complication the night after surgery.
“Now we send patients to the regular floor instead of the ICU,” say Dr. Weprin. “They still get outstanding care, but at a much lower cost.”
Could Artificial Intelligence Transform Care?
Dr. Weprin is mulling how up-and-coming tools – like virtual surgical planning and artificial intelligence – could further improve surgery and outcomes.
“There are going to be tremendous opportunities, but it’s going to take a lot of creativity and persistence to translate those into practice,” Dr. Weprin says. “We’re 100 percent committed to staying at the forefront and finding ways to give more children the chance at healthier, happier lives.”
Children’s Health is home to one of the nation’s busiest neurology and neurosurgery teams, and we’re the region’s only pediatric hospital offering techniques like open microsurgery, MRI-guided laser ablation and endovascular neurosurgery. Our specialty programs include a state-of-the-art stroke program and the only pediatric epilepsy program certified by The Joint Commission. Plus, Children’s Health’s affiliation with UT Southwestern enables a robust clinical trials program. This comprehensive care explains why U.S. News & World Report ranked our neurology and neurosurgery programs among the best of 2019-2020.
Learn more about the neurosurgery program at Children’s Health.