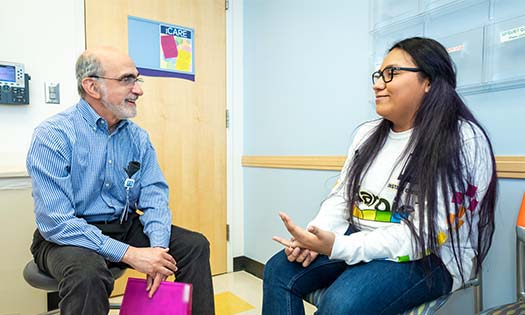The American Academy of Pediatrics (AAP) has well-known guidelines for keeping infants safe while they sleep. Though these guidelines are often reflected in hospital policy, many teams and departments fail to follow those policies strictly or consistently, putting infants at unnecessary risk of suffocation and other sleep-related death.
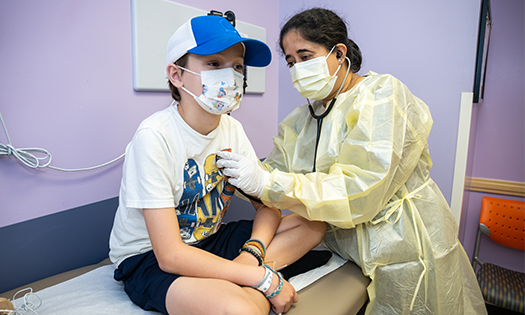
Michelle Caraballo, M.D., is leading a quality improvement initiative to ensure that staff follow the AAP guidelines for all infants up to one year old who are hospitalized at Children’s Health℠ facilities in Texas. Dr. Caraballo is a Pediatric Pulmonologist and Sleep Medicine Specialist at Children’s Health, Children’s Medical Center Dallas and Assistant Professor at UT Southwestern. Her initiative encompasses some 6,000 annual infant encounters at inpatient units across three facilities in Dallas and Plano, and includes policy changes as well as new training and educational material for nurses and parents.
Dr. Caraballo led a similar project at Children’s Hospital Colorado and has consulted with many other children’s hospitals across the U.S. Unsafe sleep practices, she has found, are the rule rather than the exception.
“Hospitals should set the standard for safe sleep,” Dr. Caraballo says. “Not only does it lower the risk of tragedy for infants under their care, it also models behavior that parents are likely to continue at home after their child is discharged.”
The Reality of Infant Sleep Practices
The Back to Sleep campaign in the 1990s lowered the rate of Sudden Infant Death Syndrome (SIDS) by 75%. But improper sleep environments remain a common danger.
“Between the ages of one month and one year, more babies die from sleep-related causes than anything else,” Dr. Caraballo says. “Many if not most of those deaths are preventable.”
The AAP recommendations include laying infants on their backs when they sleep, using a firm and flat sleep surface, dressing infants in sleep sacks or other infant clothing rather than using blankets, and placing infants alone in a crib or bassinet with no toys, pillow or other items.
Dr. Caraballo has found that hospital staff usually know these recommendations but find various reasons to depart from them. For example, they place infants on their sides in an attempt to avoid aspiration (even though the evidence does not support this). They incline the sleep surface, by stuffing something under the head area, to help the baby avoid reflux. Or they place spare diapers, wipes or other items in the crib or bassinet to make caregiving more efficient.
“These may be attempts to improve care, but in fact they introduce unnecessary risk,” Dr. Caraballo says. “Authorities review the death scene after a baby dies in their sleep, and they nearly always find that one or more safe sleep recommendations weren’t being followed.”
While babies in the hospital wear monitors that signal when the baby’s heartbeat or oxygen levels drop, babies at home don’t have that protection. And research has shown that parents often copy the infant sleep practices – good or bad – that they observe in the hospital.
Dr. Caraballo saw this firsthand with parents she interviewed for her initiative. “Parents assume whatever steps we take are the best and safest. If we cut corners, we’re telling parents something is okay when actually it isn’t.”
Laying the Groundwork for Change
To learn how infant sleep was practiced at Children’s Health, Dr. Caraballo made surprise visits to different inpatient units and observed nurses in action. She also surveyed them about their awareness of policies and level of sleep-focused training.
From there, she revised the health system’s sleep policies, bringing them more strictly in line with the latest AAP recommendations and cutting out ambiguity.
“For example, the policy used to say ‘place infants on their backs unless there’s a medical reason not to,’ which allows for too much individual discretion,” says Dr. Caraballo. “Now we list the specific situations, such as open myelomeningocele, where side or stomach sleeping is clearly necessary.”
She also changed the language around bedding, to specify that sleep sacks should be used whenever possible. If not, blankets should be lightweight and tightly tucked around the child.
“Hospitals can get free sleep sacks from the Halo company,” Dr. Caraballo explains. “Our pharmacy also sells them at cost, so parents can afford to take one home.”
Putting It Into Practice
Over time, Dr. Caraballo has enlisted and attracted a team of other advocates to join the initiative. They include members of the injury prevention department, clinical nurse managers, nurse education managers, and a child life specialist from the NICU.
“Nursing leaders are indispensable to an effort like this, because they know the needs and concerns of the floor staff better than anyone,” Dr. Caraballo says.
Together, the team helped develop and assign new training to more than 2,000 Children’s Health nurses who provide bedside care to infants. They also created an educational video available to parents through the in-room TV system.
“Every component takes approval from different people in different departments, like communications and IT,” Dr. Caraballo adds. “So, a big part of this project has been learning everyone I need to talk to in order to get things off the ground.”
Another part, she says, is perseverance. Providers eager to launch similar projects in their own health systems must commit for the long term.
“Organizations are complex, and habits die hard,” she admits. “But I just feel it’s my duty to ensure we do what’s best for every baby we care for.”
Learn more about the how experts at Children’s Health treat pediatric pulmonology conditions.